
Treating TMD: A Neuromuscular DentistÔÇÖs Domain
What is a Neuromuscular Dentist? We are! Learn more...
Research estimates that over half of the population experiences some signs and symptoms of temporomandibular joint disorder (TMD). Many of the patients who are left untreated have continuing underlying pathology that decreases the quality of their lives in subtle ways. Often patients who do not require treatment due to symptoms will opt to use neuromuscular techniques to improve function and appearance.
Neuromuscular Dentistry incorporates computers and technology to help detect and diagnose different types of TMD. Using non-invasive therapy our neuromuscular dentists can help alleviate symptoms such as headaches, neck and shoulder pain, jaw pain, clicking or popping in the jaw, and tinnitus (ringing in the ears). The majority of North Americans suffer from one or more of these symptoms, and unfortunately in many cases these patientsÔÇÖ symptoms are either misdiagnosed or dismissed as having no physiological cause.
To learn more click on the following Whiteboard Presentation, see the FAQs below about TMD and headaches, visit our Before and After page or listen to our patient Testimonials to hear about actual results.
Whiteboard Presentation
Pain is your brain's way of telling you that something is wrong. It is like a 'check engine' light that pops up in your car. It's an early warning sign that requires your attention before something more serious occurs.
Just like in the other parts of your life, science, computers, and technology are affecting your dental care. There are machines that outperform humans in basic dental services like finding cavities and machines that can measure tiny changes in your jaw tension. Neuromuscular dentistry takes a much broader view of dental health. We have found that many previously ignored factors can profoundly affect your sleep and snoring, the wearing away of your teeth and gums, your stress levels, your posture, and even your physical strength.

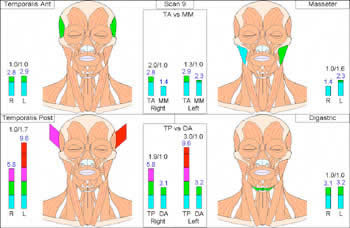
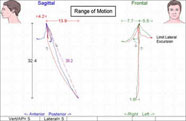

You can now see if your mouth is wide enough, if your jaw is forward enough, if your jaw moves properly, and you can see high resolution pictures of your teeth. Along with the technology has come training for dentists in neuromuscular dentistry. Neuromuscular dentists are able to both measure and correct nerve and muscle imbalances, which can lead to headaches, sub-optimal athleticism, snoring, poor posture, and tooth and jaw pain. We have two highly trained neuromuscular dentists at our office who have both achieved Fellowship status at the prestigious Las Vegas Institute for Advanced Dentistry.
FAQs
Neuromuscular Dentistry
Why is a neuromuscular orthotic so different than the "orthotic" or mouthpiece that I am already wearing?
Unfortunately, this question is all too common. By the time we meet most of our TMD/TMJ or headache patients they have already been to multiple other doctors and may even have a drawer full of "orthotics". The average number of doctors our patients have seen before walking in our door is typically between 5-8 but we have treated patients who were giving it one last try after over 20 previous doctors! Our goal, and thus far we have succeeded, is to always be the last doctor they will ever need for their TMD/TMJ or headaches.
A neuromuscular orthotic is an appliance that positions the jaw where the muscles are in a comfortable physiological position as shown on the computer and with the diagnostic data. The orthotic allows a test of this new position and allows additional healing. Other orthotics or mouth pieces that are not made to the precise neuromuscularly relaxed position are much less likely to provide consistent, profound relief over a long period of time. Also, unless the dentist is specifically trained on how to maintain the comfortable position, patients may find that the pain returns during or after orthotic wear.
Proper neuromuscular position is found with the use of the ULF-TENS, EMG readings, sonography and jaw tracking. It is in this way that neuromuscular dentists find the exact positioning for their patients' cervicomandibular region and then strictly maintain that position. This attention to physiologic harmony is what makes treatments so much more predictable and effective for a wide range of patients especially the more severe cases where other "TMJ experts" are unable to find relief. Because of the strong emphasis put on the discovery of and maintenance of the proper cervicomandibular position, Neuromuscular dentists are typically able to provide comfort over the long term. The orthotic is not the start of treatment nor is it usually the end point. Essentially, the neuromuscular orthotic is a small part of a much more detailed and meticulous form of TMJ/TMD treatment.
Why is Neuromuscular Dentistry important and is there scientific support for it's efficacy?
Dental health is affected by a triad of factors ÔÇö the teeth, the muscles and the temporomandibular joints. Traditional dentistry has focused on the teeth ÔÇö what might be called "one-dimensional" dentistry. Neuromuscular Dentistry (NMD) is a term that has been applied to the additional consideration of the "second & third dimensions" ÔÇö muscles and TM joints.
The dental curriculum prepares dentists to deal with the teeth. Muscles and joints typically get a cursory once-over. As dentists begin to practice, it is not uncommon to hear them say that they have done procedures "by the book" and yet have less than satisfactory results.
Neuromuscular Dentists commonly report that taking muscle and joint status into consideration aids them in optimizing treatment, giving them the added insight needed to treat complex cases. There is a significant body of literature published over the past 50 years that supports the efficacy of neuromuscular dental principles.
How would I know if I have a "bad bite"?
Symptoms may include:
- Tooth grinding and clenching
- Flat, worn teeth
- Chipped or broken teeth
- Retruded chin or overbite
- Short lower third of the face
- Short, square looking teeth
- Missing teeth
- Receding gums
- Cavities occurring at the gum line
- Snoring or sleep apnea
- Recurring shoulder, neck or back tension
- Ringing in the ears
- Numbness in the fingers
- Headaches
What does treatment involve?
First step is to reprogram the muscles from their habitual position to their ideal position using a low-grade stimulus. It is called ULF-TENS and is very different than a TENS from a physical therapist. This device improves blood flow and changes the metabolism of the muscles to a healthier basis. With the muscles in a resting position we can monitor and measure muscle activity and movements with computers and attached equipment. The jaw joints are also monitored to evaluate their health. Various treatments can be recommended and provided once we have the data. Treatment can include resolution of pain with dental orthotics, orthodontic movement in a body harmonic position, restorative care to ensure comfort over years, coronoplasty (adjustments to the bite), change airway and resolve breathing issues both during the day and the night. Other care is available if needed.
What is a neuromuscular orthotic?
A neuromuscular orthotic is an appliance that positions the jaw where the muscles are in a comfortable physiological position as shown on the computer and with the diagnostic data. The orthotic allows a test of this new position and allows additional healing. This diagnostic orthotic phase is also known as "phase one" of treatment.
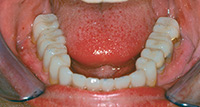
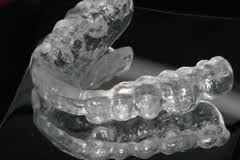
There are two main types of diagnostic orthotics that we use, fixed and removable. A fixed orthotic is bonded to the upper and/or lower teeth and does not come on and off. It is made to look like perfectly straight teeth and there are choices of different tooth colors. Fixed orthotics typically offer quicker healing and a better representation of how a patient will feel after Phase 2 or the restorative phase. A removable orthotic is an acrylic mandibular repositioner that can be taken on and off. If compliance by the patient is great then the removable orthotic can be as effective as the fixed version.
Head and Neck Pain
How do I know if I have Temporomandibular Joint Dysfunction (TMD)?
The symptoms of TMD can vary significantly from one person to the next. There are hundreds of symptoms that have been associated with TMD. Some of the more common symptoms include:
- Pain and soreness in the jaw and facial muscles
- Tooth grinding or clenching
- Clicking/popping noise in the jaw
- Ringing in the ears or feeling of congestion
- Headaches, dizziness, nervousness
- Sleep problems and/or snoring
- Neck and shoulder pain
- Tightness/ loss of range of motion in the jaw and neck
How does a joint in the jaw affect the ears and neck/shoulder area?
The jaw joint (temporomandibular joint or TMJ) is a delicately balanced mechanism. Although the joint itself is small, it is essential to many interrelated functions such as speaking, eating, and facial expressions. It is also interconnected with the musculoskeletal function as a whole. Compression of this joint from a poor bite can place pressure to nearby bones affecting balance and hearing. Compensating muscles can entrap nerves leading to referring pain or numbness to other areas of the neck and upper back regions.
How did I get TMD?
Research has not yet determined all the possible causes of TMD. We do know that TMD can be precipitated or aggravated by trauma, certain health care procedures, oral habits, and diseases such as osteoarthritis and fibromyalgia. Current research shows malocclusion (poor positioning of the lower jaw) can be a major contributing factor to TMD. Resolving this malocclusion can provide relief and healing.
Is TMD treatable?
TMD is treatable by well-trained neuromuscular dentists. Treatment consists of a thorough evaluation and assessment. Oral appliances are often recommended. Permanent solutions such as orthodontics or dental restorations may be indicated.
Can I just live with TMD as I have been and hope it goes away?
TMD will not go away on its own. As your body tries to accommodate the problems associated with it, it can actually become worse. In the vast majority of cases, TMD, if left untreated will continue to progress, causing pain, damage to your jaw and neck, tooth damage, and loss of bone and teeth.
Is TMD common?
Yes, approximately ten million people in the United States have TMD at any given time, according to the National Institute of Dental and Craniofacial Research. Many people go undiagnosed or are misdiagnosed with migraine headaches, Meniere's disease, depression, or other unrelated issues.
Does insurance cover treatment?
Insurance companies debate whether it is a medical, dental, or psychological issue. This shows the lack of information regarding the whole issue and the inability of the health communities to help treat the ÔÇ£wholeÔÇØ person under a single diagnosis. There are medical billing codes for these conditions/treatments and can be provided to you in your attempt to get benefits. We encourage you to check with your particular medical insurance carrier.
Headaches
How can your bite cause a headache?
Tension headaches result from muscle strain, or contraction. When muscles are held tight for long periods of time they begin to ache. Headaches from dental stress are a type of muscle tension headache. A tension headache may be on one or both sides of your head. Or, it may surround your head as if a steel band were wrapped around it. The pain feels like a dull, non-throbbing ache. Specific signs which indicate that the headache may have a dental origin include:
- Pain behind the eyes
- Sore jaw muscles or "tired" muscles upon awakening
- Teeth grinding
- Clicking or popping jaw joints
- Head and/or scalp painful to the touch
Why do my jaw muscles ache?
Muscles that control your jaw and hold your head upright are very complex both in number and interactions. Every time you swallow, your upper and lower teeth must come together in a firm way to brace the jaw against the skull. We swallow several hundred times a day! If your bite is unstable or the lower jaw is not in correct neuromuscular alignment, the muscles must work harder to bring the teeth together. You can rest when your body is tired but your jaw muscles never get a break! Overworked muscles become strained. When muscles are under constant strain, pain results.
How can a "bad bite" affect other muscles far from the teeth?
Your head is delicately balanced on top of your spinal column by muscles in your jaw, neck, shoulders, and back. Your head weighs approximately 16 pounds the weight of a very heavy bowling ball. Imagine your head as a bowling ball balanced on top of a pencil by a number of rubber bands. When muscles are tense, they shorten. Now imagine shortening just one of those rubber bands. Some rubber bands would stretch, some would shorten, and the bowling ball would be thrown off kilter. Similarly, when even a single jaw, neck, or shoulder muscle becomes shortened, all of the other muscles are forced to overwork to keep the head balanced on top of the spinal column. We see then that dental headaches originate from the lower jaw being held in an unstable position by a "bad bite", which causes the muscles of the jaw, head, and neck to overwork with pain and dysfunction resulting. The pain makes you feel tense and uptight. This worsens the muscle spasm, which in turn increases the pain.
Neck
Why are my fingers numb?
As the neck muscles try to maintain balance for a poor position of the head and jaw they tighten for long periods of time. This puts pressure on nerves that travel through these muscles. The entrapment of the nerves causes them to stop transmitting and you get a numb feeling.
Can a chiropractor help my neck?
A: Yes, many chiropractors can relieve symptoms. Dr. Gill and Dr. Erickson, as neuromuscular dentists, in conjunction with certain types of chiropractors or other physical therapists work to fix problems long term. Using their data and treatment conclusions allows a neuromuscular dentist to develop a long-term solution. The goal is to find the underlying cause of the problem and determine the best way to fix it permanently.
